New
Drug-resistant Tuberculosis Strains Could Become Widespread
 | The
emergence of new forms of tuberculosis (TB)
could significantly increase the proportion of drug-resistant cases globally,
according to a recent study conducted by Australian researchers at the University
of New South Wales and the University of Western Sydney. Results were published
August 12, 2009 in the Proceedings of the National Academy of Sciences.
|
Chest
X-ray image.
One in three humans already carries the TB bacterium. |
| 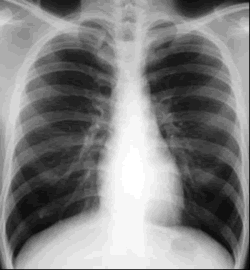 | (Credit:
Image courtesy of
University of New South Wales) |
Although
the overall incidence of TB is falling in some regions, the emergence of antibiotic
resistance could lead to the widespread emergence of untreatable strains of the
disease.
Following are edited excerpts from a review of the recent study
published in Science Daily.
Laboratory-based studies have suggested
that antibiotic-resistant TB strains cause longer-lasting infections, but with
a lower transmission rate. Therefore, scientists have questioned whether drug-resistant
TB strains are more likely than drug-sensitive strains to persist and spread --
an important question for predicting the future impact of the disease.
One
in three people already carries the TB bacterium. Although it remains latent in
most cases, the World Health Organization (WHO) has estimated there were 9.27
million new cases of TB in 2007. There were 1.6 million TB-related deaths in 2005.
Drug-resistant TB is caused by inconsistent or partial treatment, when patients
do not take all their medicines regularly for the required period or because the
drug supply is unreliable.
A research team led by University of New South
Wales' Dr. Mark Tanaka used epidemiological and molecular data from Mycobacterium
tuberculosis strains isolated from Cuba, Estonia, and Venezuela to estimate
the rate of evolution of drug resistance and to compare the relative "reproductive
fitness" of resistant and drug-sensitive strains.
"We found that
the overall fitness of drug-resistant strains is comparable to drug-sensitive
strains," said Dr. Tanaka of the Evolution and Ecology Research Centre. "This
was especially so in Cuba and Estonia, where the there is a high prevalence of
drug-resistant cases."
The finding may reflect an inconsistency in
drug treatment programs in these countries. Indeed, Estonia now has one of the
highest rates of multi-drug resistant TB in the world. The intermittent presence
of drugs and the resulting transmission of resistant strains would have let drug-resistant
strains collectively spend more time within untreated hosts, allowing them to
evolve ways to become more infectious and out-compete the drug-sensitive strains.
The
study also reveals that the contribution of transmission to the spread of drug
resistance is very high -- up to 99% -- compared with acquired resistance due
to treatment failure. "Our results imply that drug-resistant strains of TB
are likely to become highly prevalent in the next few decades," said UNSW's
Dr. Fabio Luciani, the study's lead author. "They also suggest that limiting
further transmission of TB might be an effective approach to reducing the impact
of drug resistance."
"Mathematical and statistical methods can
add a lot of value to empirical data by allowing us to account for the processes
behind them," said research co-author, Dr Andrew Francis from the University
of Western Sydney. "In this case, we use samples of TB genotypes, together
with information about drug resistance, to make inferences and predictions that
wouldn't have been possible just a few years ago."
About
TuberculosisTuberculosis
is a contagious disease. Like the common cold, it spreads through the air. Only
people who are sick with TB in their lungs are infectious. When infectious people
cough, sneeze, talk or spit, they propel TB germs, known as bacilli, into the
air. A person needs only to inhale a small number of these to be infected.
Left
untreated, each person with active TB disease will infect on average between 10
and 15 people every year. However, people infected with TB bacilli will not necessarily
become sick with the disease. The immune system "walls off" the TB bacilli
and it can lie dormant for years. When someone's immune system is weakened, however,
the chances of becoming sick are greater.
Until 50 years ago, there were
no medications to cure TB. Now, strains that are resistant to antibiotics have
emerged and about 1.7% of cases worldwide have multidrug-resistant disease (MDR-TB).
In 2006, extensively drug-resistant tuberculosis (XDR-TB) emerged. XDR-TB is defined
as MDR-TB plus resistance to any fluoroquinolone and at least one injectable agent:
kanamycin, amikacin or capreomycin. The spread of XDR-TB globally has been fuelled
by the HIV epidemic, inadequate public health systems, limited access to high-quality
laboratory resources, and a neglect of infection control measures.
[Editor's
Note]: Tibotec Therapeutic's experimental agent TMC207 has shown
promising activity against multidrug-resistant TB in a recent
study.
8/18/09
Source
D Gaffney. New Drug-resistant
TB Strains Could Become Widespread, Says New Study. Science Daily (www.ScienceDaily.com).
August 12, 2009. (Adapted from materials provided by University of New South Wales.)
Reference
F Luciania, SA Sisson, H Jiangb, and others. The epidemiological fitness
cost of drug resistance in Mycobacterium tuberculosis. Proceedings of the National
Academy of Sciences (PNAS). August 13, 2009 [Epub before print]. (Abstract).
|
| | | | Entry
Inhibitors
(including Fusion Inhibitors) |  Fuzeon
(enfuvirtide,
T-20) Fuzeon
(enfuvirtide,
T-20)
 Selzentry
(maraviroc) Selzentry
(maraviroc) |
| | |
|